- Hypohidrotic ectodermal dysplasia
-
Hypohidrotic ectodermal dysplasia Classification and external resources ICD-10 Q82.4 ICD-9 757.31 OMIM 305100 224900, 129490 DiseasesDB 29810 Hypohidrotic ectodermal dysplasia (also known as "Anhidrotic ectodermal dysplasia," and "Christ-Siemens-Touraine syndrome"[1]:570) is one of about 150 types of ectodermal dysplasia in humans. Before birth, these disorders result in the abnormal development of structures including the skin, hair, nails, teeth, and sweat glands.[2]:515-517
Contents
Presentation
 Actor Michael Berryman displays outward symptoms of the condition.
Actor Michael Berryman displays outward symptoms of the condition.
Most people with hypohidrotic ectodermal dysplasia have a reduced ability to sweat (hypohidrosis) because they have fewer sweat glands than normal or their sweat glands do not function properly. Sweating is a major way that the body controls its temperature; as sweat evaporates from the skin, it cools the body. An inability to sweat can lead to a dangerously high body temperature hyperthermia, particularly in hot weather. In some cases, hyperthermia can cause life-threatening medical problems.
Affected individuals tend to have sparse scalp and body hair (hypotrichosis). The hair is often light-coloured, brittle, and slow-growing. This condition is also characterized by absent teeth (hypodontia) or teeth that are malformed. The teeth that are present are frequently small and pointed.
Hypohidrotic ectodermal dysplasia is associated with distinctive facial features including a prominent forehead, thick lips, and a flattened bridge of the nose. Additional features of this condition include thin, wrinkled, and dark-colored skin around the eyes; chronic skin problems such as eczema; and a bad-smelling discharge from the nose (ozena).
Hypohidrotic ectodermal dysplasia is the most common form of ectodermal dysplasia in humans. It is estimated to affect at least 1 in 17,000 people worldwide.
Genetics
Mutations in the EDA, EDAR, and EDARADD genes cause hypohidrotic ectodermal dysplasia. The EDA, EDAR, and EDARADD genes provide instructions for making proteins that work together during embryonic development. These proteins form part of a signaling pathway that is critical for the interaction between two cell layers, the ectoderm and the mesoderm. In the early embryo, these cell layers form the basis for many of the body's organs and tissues. Ectoderm-mesoderm interactions are essential for the formation of several structures that arise from the ectoderm, including the skin, hair, nails, teeth, and sweat glands.
Hypohidrotic ectodermal dysplasia has several different inheritance patterns.
EDA (X-linked)
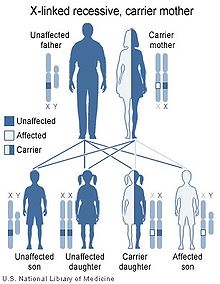
Most cases are caused by mutations in the EDA gene, which are inherited in an X-linked recessive pattern. A condition is considered X-linked if the mutated gene that causes the disorder is located on the X chromosome, one of the two sex chromosomes. In males (who have only one X chromosome), one altered copy of the gene in each cell is sufficient to cause the condition. In females (who have two X chromosomes), a mutation must be present in both copies of the gene to cause the disorder. Males are affected by X-linked recessive disorders much more frequently than females. A striking characteristic of X-linked inheritance is that fathers cannot pass X-linked traits to their sons.
In X-linked recessive inheritance, a female with one altered copy of the gene in each cell is called a carrier. In about 70 percent of cases, carriers of hypohidrotic ectodermal dysplasia experience some features of the condition. These signs and symptoms are usually mild and include a few missing or abnormal teeth, sparse hair, and some problems with sweat gland function. Some carriers, however, have more severe features of this disorder.
EDAR or EDARADD (autosomal)
Less commonly, hypohidrotic ectodermal dysplasia results from mutations in the EDAR or EDARADD gene. EDAR mutations can have an autosomal dominant or autosomal recessive pattern of inheritance, and EDARADD mutations have an autosomal recessive pattern of inheritance. Autosomal dominant inheritance means one copy of the altered gene in each cell is sufficient to cause the disorder. Autosomal recessive inheritance means two copies of the gene in each cell are altered. Most often, the parents of an individual with an autosomal recessive disorder are carriers of one copy of the altered gene but do not show signs and symptoms of the disorder.
Notable individuals
- Michael Berryman, Saturn Award-nominated character actor
See also
- Hermann Werner Siemens
- List of cutaneous conditions
- Albert Touraine
References
- ^ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0721629210.
- ^ Freedberg, et al. (2003). Fitzpatrick's Dermatology in General Medicine. (6th ed.). McGraw-Hill. ISBN 0-07-138076-0.
External links
- GeneReview/NIH/UW entry on Hypohidrotic Ectodermal Dysplasia
- Hypohidrotic ectodermal dysplasia at NLM Genetics Home Reference
- Author Web Site for Bonnie J. Rough, whose award-winning memoir "Carrier: Untangling the Danger in My DNA" describes one family's experience with hypohidrotic ectodermal dysplasia
- Bonnie J. Rough speaks about her family's history with HED on KRUI's The Lit Show
Congenital malformations and deformations of integument / skin disease (Q80–Q82, 757.0–757.3) Genodermatosis Congenital ichthyosis/
erythrokeratodermiaADARUngroupedIchthyosis bullosa of Siemens · Ichthyosis follicularis · Ichthyosis prematurity syndrome · Ichthyosis–sclerosing cholangitis syndrome · Nonbullous congenital ichthyosiform erythroderma · Ichthyosis linearis circumflexa · Ichthyosis hystrixEB
and relatedJEB (JEB-H, Mitis, Generalized atrophic, JEB-PA)related: Costello syndrome · Kindler syndrome · Laryngoonychocutaneous syndrome · Skin fragility syndrome ·Naegeli syndrome/Dermatopathia pigmentosa reticularis · Hay–Wells syndrome · Hypohidrotic ectodermal dysplasia · Focal dermal hypoplasia · Ellis–van Creveld syndrome · Rapp–Hodgkin syndrome/Hay–Wells syndromeEhlers–Danlos syndrome · Cutis laxa (Gerodermia osteodysplastica) · Popliteal pterygium syndrome · Pseudoxanthoma elasticum · Van Der Woude syndromeHyperkeratosis/
keratinopathydiffuse: Diffuse epidermolytic palmoplantar keratoderma • Diffuse nonepidermolytic palmoplantar keratoderma • Palmoplantar keratoderma of Sybert • Mal de Meleda •syndromic (connexin (Bart–Pumphrey syndrome • Clouston's hidrotic ectodermal dysplasia • Vohwinkel syndrome) • Corneodermatoosseous syndrome • plakoglobin (Naxos syndrome) • Scleroatrophic syndrome of Huriez • Olmsted syndrome • Cathepsin C (Papillon–Lefèvre syndrome • Haim–Munk syndrome) • Camisa diseasefocal: Focal palmoplantar keratoderma with oral mucosal hyperkeratosis • Focal palmoplantar and gingival keratosis • Howel–Evans syndrome • Pachyonychia congenita (Pachyonychia congenita type I • Pachyonychia congenita type II) • Striate palmoplantar keratoderma • Tyrosinemia type II)punctate: Acrokeratoelastoidosis of Costa • Focal acral hyperkeratosis • Keratosis punctata palmaris et plantaris • Keratosis punctata of the palmar creases • Schöpf–Schulz–Passarge syndrome • Porokeratosis plantaris discreta • Spiny keratodermaungrouped: Palmoplantar keratoderma and spastic paraplegia • desmoplakin (Carvajal syndrome) • connexin (Erythrokeratodermia variabilis • HID/KID)OtherMeleda disease · Keratosis pilaris · ATP2A2 (Darier's disease) · Dyskeratosis congenita · Lelis syndromeDyskeratosis congenita · Keratolytic winter erythema · Keratosis follicularis spinulosa decalvans · Keratosis linearis with ichthyosis congenital and sclerosing keratoderma syndrome · Keratosis pilaris atrophicans faciei · Keratosis pilarisOthercadherin (EEM syndrome) · immune system (Hereditary lymphedema, Mastocytosis/Urticaria pigmentosa) · Hailey–Hailey
see also Template:Congenital malformations and deformations of skin appendages, Template:Phakomatoses, Template:Pigmentation disorders, Template:DNA replication and repair-deficiency disorderDevelopmental
anomaliesMidlineOther/ungroupedAplasia cutis congenita · Amniotic band syndrome · Branchial cyst · Cavernous venous malformation
Accessory nail of the fifth toe · Bronchogenic cyst · Congenital cartilaginous rest of the neck · Congenital hypertrophy of the lateral fold of the hallux · Congenital lip pit · Congenital malformations of the dermatoglyphs · Congenital preauricular fistula · Congenital smooth muscle hamartoma · Cystic lymphatic malformation · Median raphe cyst · Melanotic neuroectodermal tumor of infancy · Mongolian spot · Nasolacrimal duct cyst · Omphalomesenteric duct cyst · Poland anomaly · Rapidly involuting congenital hemangioma · Rosenthal–Kloepfer syndrome · Skin dimple · Superficial lymphatic malformation · Thyroglossal duct cyst · Verrucous vascular malformation · BirthmarkDeficiencies of intracellular signaling peptides and proteins GTP-binding protein regulators GTPase-activating proteinMarinesco–Sjögren syndrome · Aarskog–Scott syndrome · Juvenile primary lateral sclerosis · X-Linked mental retardation 1G protein cAMP/GNAS1: Pseudopseudohypoparathyroidism · Progressive osseous heteroplasia · Pseudohypoparathyroidism · Albright's hereditary osteodystrophy · McCune–Albright syndrome
CGL 2RAS: HRAS (Costello syndrome) · KRAS (Noonan syndrome 3, KRAS Cardiofaciocutaneous syndrome)
RAB: RAB7 (Charcot–Marie–Tooth disease) · RAB23 (Carpenter syndrome) · RAB27 (Griscelli syndrome type 2)
RHO: RAC2 (Neutrophil immunodeficiency syndrome)
ARF: SAR1B (Chylomicron retention disease) ARL13B (Joubert syndrome 8) · ARL6 (Bardet–Biedl syndrome 3)MAP kinase Other kinase/phosphatase RPS6KA3 (Coffin-Lowry syndrome) · CHEK2 (Li-Fraumeni syndrome 2) · IKBKG (Incontinentia pigmenti) · STK11 (Peutz–Jeghers syndrome) · DMPK (Myotonic dystrophy 1) · ATR (Seckel syndrome 1) · GRK1 (Oguchi disease 2) · WNK4/WNK1 (Pseudohypoaldosteronism 2)PTEN (Bannayan–Riley–Ruvalcaba syndrome, Lhermitte–Duclos disease, Cowden syndrome, Proteus-like syndrome) · MTM1 (X-linked myotubular myopathy) · PTPN11 (Noonan syndrome 1, LEOPARD syndrome, Metachondromatosis)Signal transducing adaptor proteins Other NF2 (Neurofibromatosis type II) · NOTCH3 (CADASIL) · PRKAR1A (Carney complex) · PRKAG2 (Wolff–Parkinson–White syndrome) · PRKCSH (PRKCSH Polycystic liver disease) · XIAP (XIAP2)Genetic disorder, membrane: cell surface receptor deficiencies G protein-coupled receptor
(including hormone)Class ATSHR (Congenital hypothyroidism 1) · LHCGR (Male-limited precocious puberty) · FSHR (XX gonadal dysgenesis) · EDNRB (ABCD syndrome, Waardenburg syndrome 4a, Hirschsprung's disease 2) · AVPR2 (Nephrogenic diabetes insipidus 1) · PTGER2 (Aspirin-induced asthma)Class BClass CCASR (Familial hypocalciuric hypercalcemia)Class FFZD4 (Familial exudative vitreoretinopathy 1)Enzyme-linked receptor
(including
growth factor)ROR2 (Robinow syndrome) · FGFR1 (Pfeiffer syndrome, KAL2 Kallmann syndrome) · FGFR2 (Apert syndrome, Antley-Bixler syndrome, Pfeiffer syndrome, Crouzon syndrome, Jackson-Weiss syndrome) · FGFR3 (Achondroplasia, Hypochondroplasia, Thanatophoric dysplasia, Muenke syndrome) · INSR (Donohue syndrome · Rabson–Mendenhall syndrome) · NTRK1 (Congenital insensitivity to pain with anhidrosis) · KIT (KIT Piebaldism, Gastrointestinal stromal tumor)JAK-STAT TNF receptor Lipid receptor LRP: LRP2 (Donnai-Barrow syndrome) · LRP4 (Cenani Lenz syndactylism) · LRP5 (Worth syndrome, Familial exudative vitreoretinopathy 4, Osteopetrosis 1)
LDLR (LDLR Familial hypercholesterolemia)Other/ungrouped Immunoglobulin superfamily: AGM3, 6
Integrin: LAD1 · Glanzmann's thrombasthenia · Junctional epidermolysis bullosa with pyloric atresia
EDAR (EDAR Hypohidrotic ectodermal dysplasia) · PTCH1 (Nevoid basal cell carcinoma syndrome) · BMPR1A (BMPR1A Juvenile polyposis syndrome) · IL2RG (X-linked severe combined immunodeficiency)Cytokine EDA Hypohidrotic ectodermal dysplasia · Camurati-Engelmann diseaseEphrin WNT Tetra-amelia syndromeTGF Fas ligand Endothelin Other DHH (DHH XY gonadal dysgenesis) · BMP15 (Premature ovarian failure 4) · TSHB (Congenital hypothyroidism 4)Categories:- Genodermatoses
- Defects in innate immunity
Wikimedia Foundation. 2010.